Arthritis Rheumatol:痛风,如何用药效果更好?
2017-06-12 枫丹白露 来宝网
在324例腹痛患者的III期临床试验中,与芬布斯他汀联合使用的药物维生素在降低尿酸血症水平方面比单独使用氟比斯坦更好。超过12个月的实验观察之后,联合药物组合组的使用患者中,已经有显着多的患者达到目标水平的尿酸盐,这比单用芬布斯他汀组效果更明显。
在324例腹痛患者的III期临床试验中,与芬布斯他汀联合使用的药物维生素在降低尿酸血症水平方面比单独使用氟比斯坦更好。超过12个月的实验观察之后,联合药物组合组的使用患者中,已经有显着多的患者达到目标水平的尿酸盐,这比单用芬布斯他汀组效果更明显。
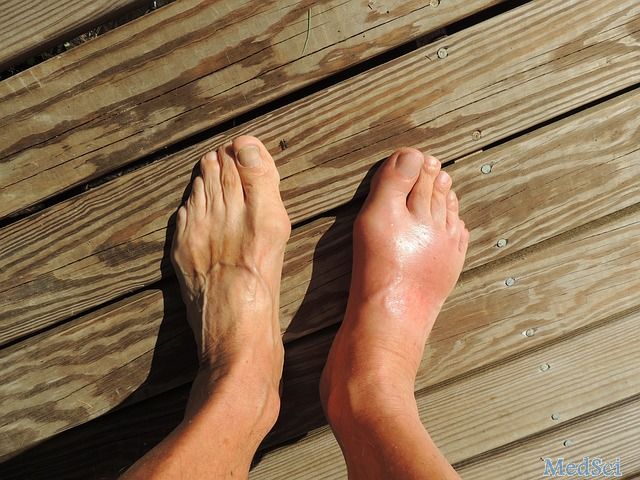
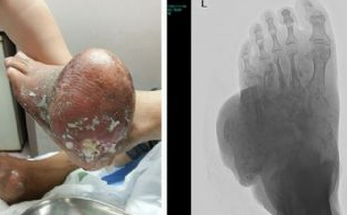
当尿酸盐晶体积聚在关节中时,发生痛风,引起炎症和剧烈疼痛。在一些人中,形成大量的尿酸盐晶体沉积物(tophi)。这些沉积物可引起慢性关节炎症和损伤。目前针对痛风长期治疗的指南,建议使用降脂治疗方法,以维持腹痛患者血尿酸水平低于5.0 mg / dl。推荐的一线降尿酸治疗药物是黄嘌呤氧化酶抑制剂,别嘌呤醇或芬布斯他汀,抑制尿酸盐的产生。然而,许多患者不能用这些药物达到<5.0mg / dl的尿酸盐水平。
莱西诺拉德抑制肾脏中的尿酸转运蛋白,并增加尿液中尿酸的排泄。因此,与黄嘌呤氧化酶抑制剂组合的病毒素提供了通过增加肾脏排泄尿酸并减少尿酸盐产生来降低尿酸血液水平的双重作用机制。
关节炎和风湿病学试验的主要作者Nicola Dalbeth教授说:“莱西诺拉德和芬布斯他汀的联合治疗代表了严重痛风患者不能达到黄嘌呤氧化酶抑制剂单一疗法的血清尿酸盐治疗目标的新治疗选择。
原始出处:
Nicola Dalbeth, Graeme Jones, et al. Lesinurad, a Selective Uric Acid Reabsorption Inhibitor, in Combination With Febuxostat in Patients With Tophaceous Gout: A Phase III Clinical Trial. Arthritis & Rheumatology Accepted manuscript online: 9 June 2017 DOI: 10.1002/art.40159
版权声明:
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言







#Arthritis#
53
#药效#
95
#ART#
80
文章不错,拜读了
92
学习了,涨知识
96